
At the University of Washington School of Nursing, the end of the spring quarter is never just one moment.
There are the events that everyone sees: Nurse Week celebrations, school-wide announcements, and ceremonies from Kane Hall to Alaska Airlines Arena. Then there are the quieter moments that exist between students and faculty: the last clinical shift, the last exam, the last time walking into the Health Sciences Building as a student rather than a professional.
Nursing school is hard. It comes with a daily juggle of scheduling meals or snacks between lectures, clinical rotations, and simulation lab time, studying for exams that demand not just knowledge but judgment under pressure, and long days that turn into longer nights, often filled with questions and doubt. Students apply to our programs knowing the rigor on an intellectual level, but as the quarters continue to move forward, the impact of that knowing becomes more real.
Then, as summer begins to peek through the greyness unique to Seattle’s winter skies, students approaching the end of their program help usher in the sun. As posts about the upcoming graduation begin to fill our social media tags, they bring with them the promise of summer break, preparation for NCLEX testing and national boards, and every earned moment of what comes when you shine with the brightness of accomplishment.
This year, the School of Nursing is calling the final weeks of May and the first weeks of June exactly what they are: a season of celebration — and we welcome you to join us.
Celebration traditions that span the centuries: The Nursing Pinning Ceremony
The nursing pin carries roots that trace back to the 12th century, when monks who cared for sick and injured Crusaders were recognized with a Maltese cross — a symbol of service, devotion, and belonging to a community of care. By 1916, that tradition had grown into the pinning ceremony practiced in nursing schools across the country.
Each year, the UW School of Nursing holds pinning ceremonies for graduates in August, March, and June. This unique experience does not serve as a marker of the moment a student becomes a nurse- graduation and licensure do that; pinning marks something more personal; the choice each scholar made to walk this path, the commitment they’ve shown year after year, and the gratitude they feel toward those who stood alongside them. It is the only ceremony in a nurse’s education designed entirely around recognition, not of an institution, but of a journey, and the community that made it possible.
Hilaire J. Thompson, Robert G. and Jean A. Reid Executive Dean of the UW School of Nursing, reflected on her ABSN pinning — and on what makes the UW tradition distinct.
“My own pinning was in 1992 at the Catholic University of America. It was a formal ceremony for the BSN and ABSN students, held in the performing arts theatre on campus. The associate dean for students pinned each of us, while our faculty, family, and friends gathered to celebrate… What I love about the UW tradition is that our students choose their own pinner — and sometimes more than one. They get to honor the people who carried them through: a parent, a partner, a mentor, a faculty member, a friend. That single choice turns the ceremony from a formality into something deeply personal. It says, in front of everyone, here is who walked with me. That, to me, is what pinning is for.”
— Hilaire J. Thompson, Robert G. and Jean A. Reid Executive Dean, UW School of Nursing

A celebration “omnes una”: The UW School of Nursing Convocation
The Latin word convocare means to call together, and at the UW School of Nursing, we look forward to calling forward our community to celebrate a job well done. From families and friends who gave understanding and support to the trusted faculty who taught and challenged our scholars each day, and advisors, coordinators, and staff whose steady, often invisible work helped them to stay on track- this is the moment all of us come together to say to our graduates: you are ready, and we are with you.
“As we walk into Hec Edmundson Pavilion this year as a SoN community, each of us brings a sense of joy and accomplishment. As a school, we choose to take time to reflect on and thank those who helped make this moment possible, and I want to encourage our graduates to do the same. It is my hope that they take with them not only the knowledge and skills gained from their programs, but the commitment we hold near to us as the University of Washington School of Nursing, to care for and advocate for a healthcare system that serves all.”
— Hilaire J. Thompson, Robert G. and Jean A. Reid Executive Dean, UW School of Nursing

Fifty-five years of preparing what’s next
This year’s celebration carries an extra layer of meaning.
In 1971, the University of Washington launched PRIMEX — one of the first family nurse practitioner programs in the country. Its premise, though now considered foundational, was deemed radical at the time, based on the belief that nurses, given the right preparation and authority, could serve as primary care providers for patients who remained unserved and without basic healthcare access.
Fifty-five years later, that premise has held. Patients in rural and historically marginalized communities still rely on nurse practitioners for accessible, responsive care. What began as a single program has grown into the graduate and advanced practice education system that defines the UW School of Nursing today, including the first DNP program on the West Coast, and now, the #1-ranked public DNP program in the country.
A class Washington has been waiting for
Thousands of graduates have gone on to lead health improvements at the local, national, and global levels since the first nursing course was introduced at the University of Washington in 1916, and now, graduates are joining a healthcare workforce that desperately needs them.
Without intervention, Washington is projected to have the nation’s largest nursing shortage by 2037. This year, as we have done so many years before, the University of Washington School of Nursing will send nurses, nurse practitioners, nurse-midwives, nurse leaders, clinical informaticists, and nursing scientists, researchers, and innovators into hospitals, clinics, community health centers, and research institutions across the world, ready to practice compassionate, cutting edge care as trained professionals capable of leading change in the healthcare ecosystem.
This is, and always has been, the legacy of the University of Washington School of Nursing.
Join us in celebrating
Whether you are a proud family member, a longtime friend of the school, a prospective student, or simply someone who wants to celebrate what UW Nursing represents, you are welcome.
SoN Convocation & Awards Ceremony
Friday, June 5, 2026 | 6–8 p.m.
Alaska Airlines Arena at Hec Edmundson Pavilion
Doors open at 5 p.m. for student check-in.
All are welcome, and we hope to see you there. A livestream will be available for those who cannot attend in person.
To learn more about UW School of Nursing programs, research, and community, visit nursing.uw.edu.


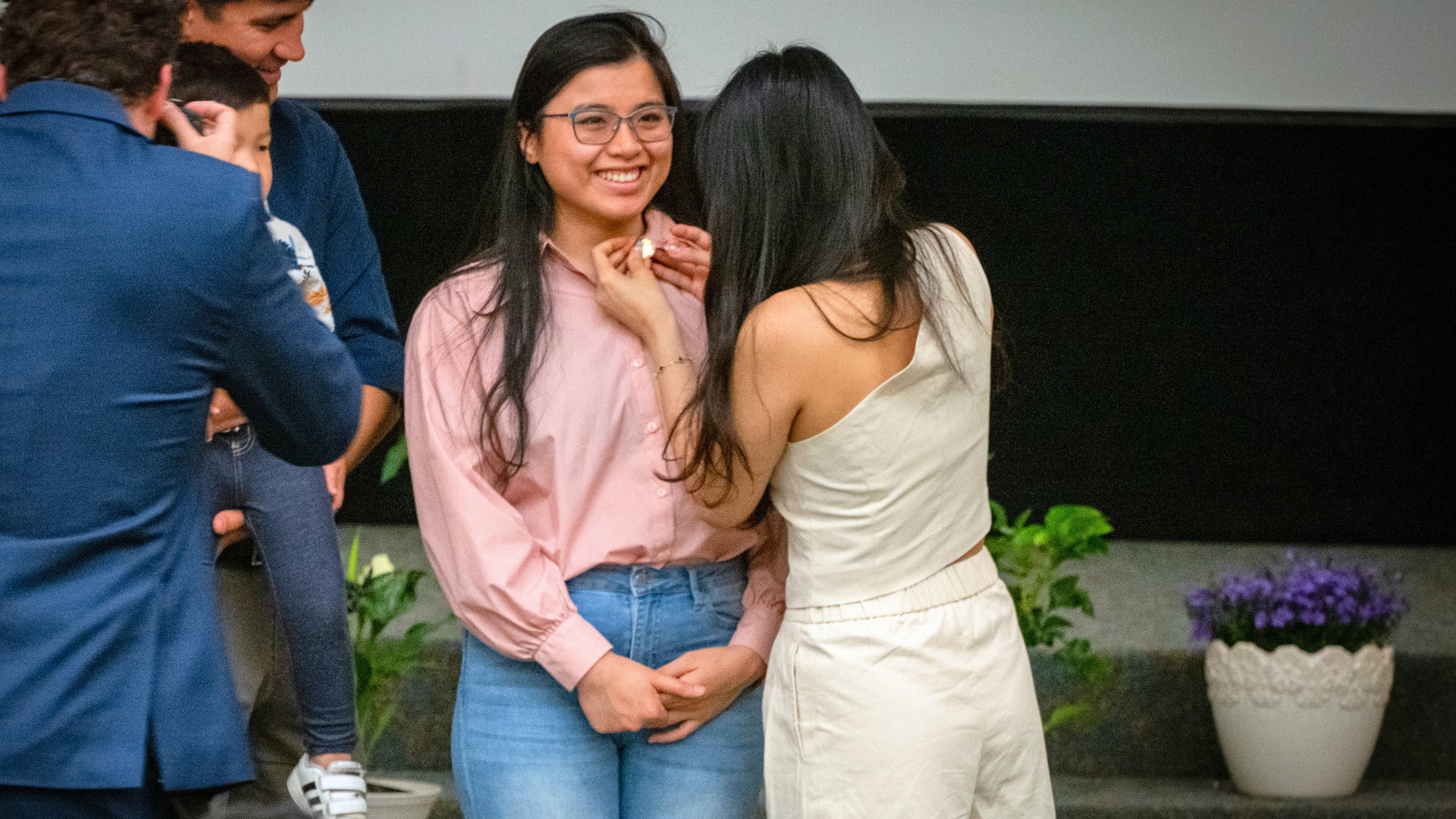































 That same spirit of leadership continues in students like Marin Strong, a PhD in Nursing Science student whose recent appointment as a Sigma United Nations Youth Representative reflects not only personal achievement, but history in the making.
That same spirit of leadership continues in students like Marin Strong, a PhD in Nursing Science student whose recent appointment as a Sigma United Nations Youth Representative reflects not only personal achievement, but history in the making.



 Suah Park is a PhD in Nursing Science candidate and one of the de Tornyay Center’s 2025-2026 Healthy Aging Scholars. Her faculty mentor is
Suah Park is a PhD in Nursing Science candidate and one of the de Tornyay Center’s 2025-2026 Healthy Aging Scholars. Her faculty mentor is 
 Mary Eliza Mahoney was the first African American to graduate from an American nursing program in 1879. She worked to improve access and professional standards for African American nurses and was a co-founder of the National Association of Colored Graduate Nurses.
Mary Eliza Mahoney was the first African American to graduate from an American nursing program in 1879. She worked to improve access and professional standards for African American nurses and was a co-founder of the National Association of Colored Graduate Nurses.



 Rachel Suggs Pitts, BSN ’56,
Rachel Suggs Pitts, BSN ’56, Lois Price Spratlen, BSN ’76,
Lois Price Spratlen, BSN ’76,



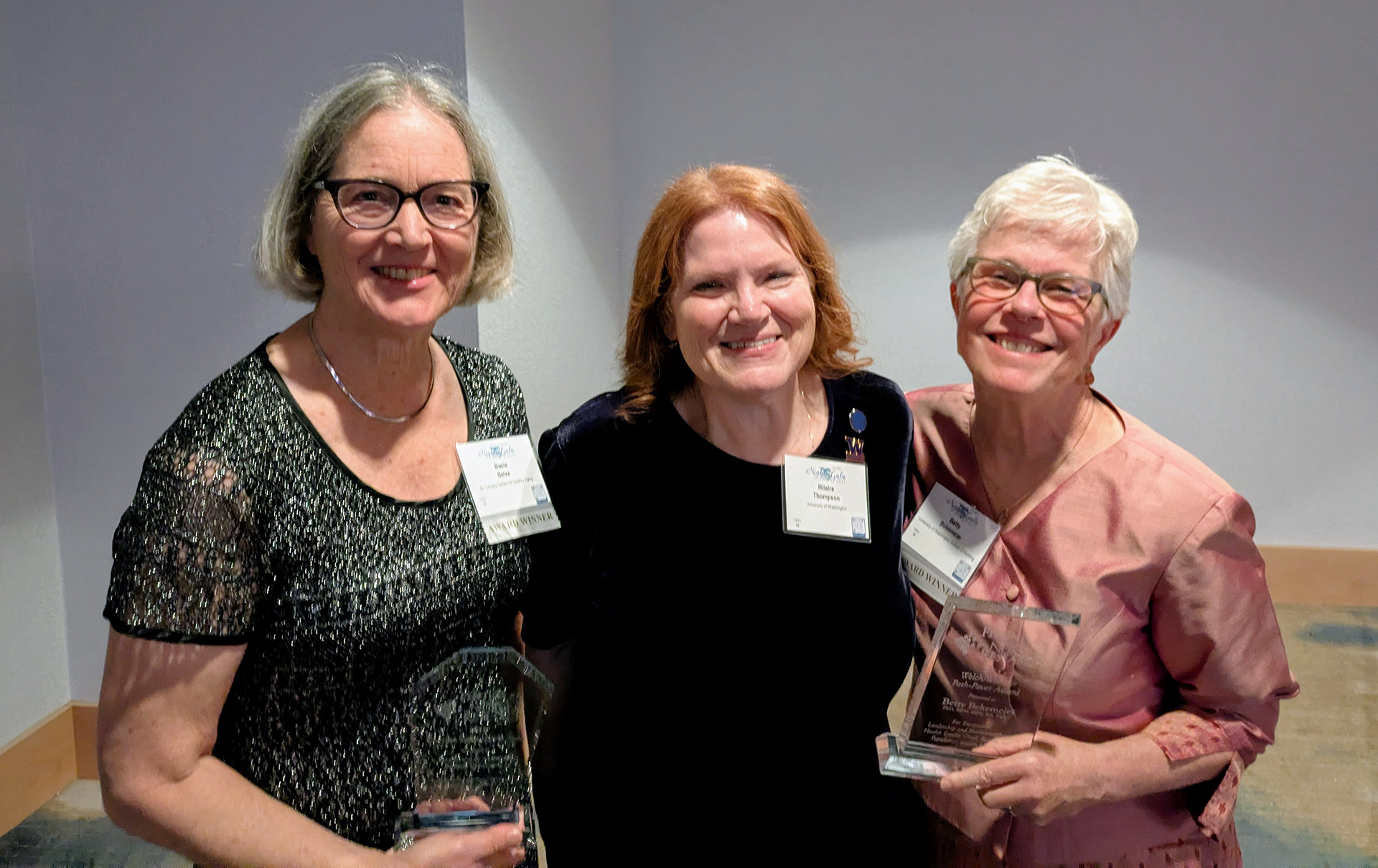






 Effective April 1, 2025,
Effective April 1, 2025, 














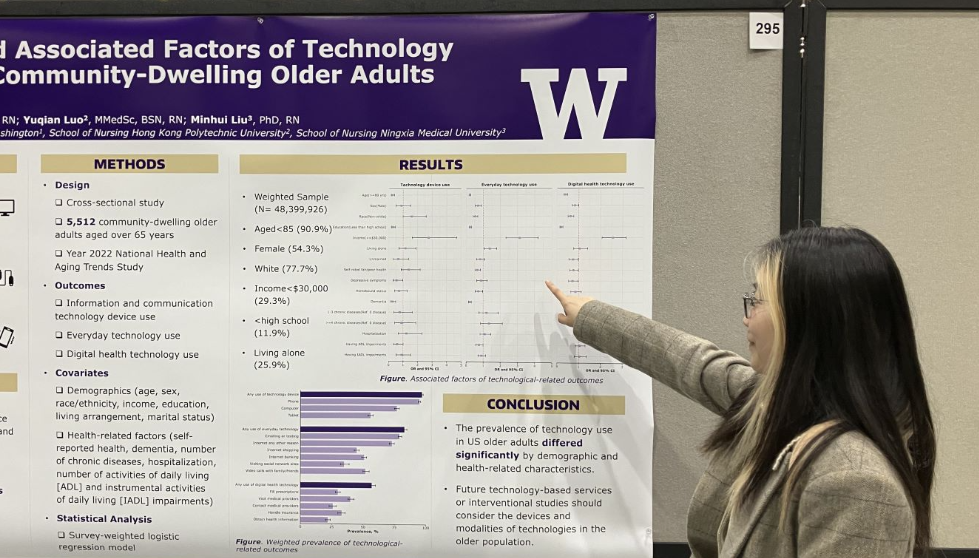

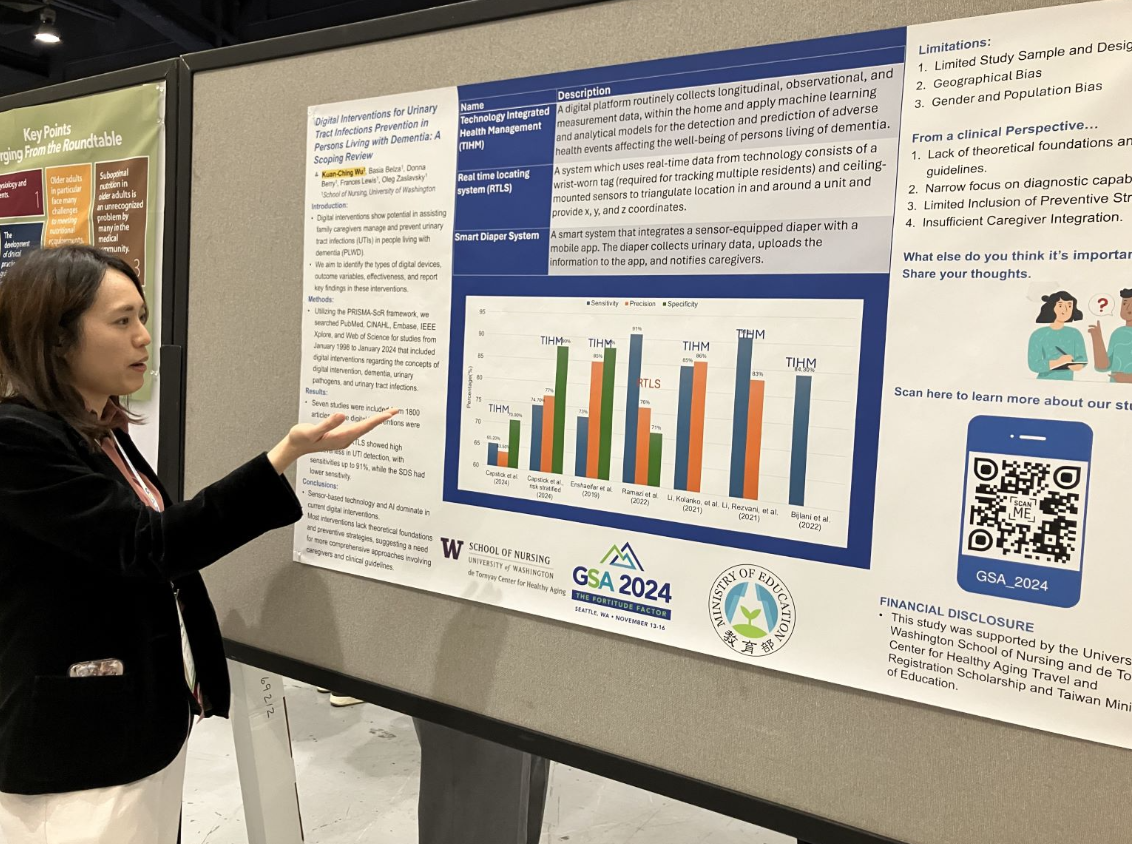






 Welsch served as a Person-centered Care Coach on project in Washington State spearheaded by the Alzheimer’s Association. The project aimed to help long-term care facilities improve quality care for people living with Alzheimer’s and dementia by implementing the Alzheimer’s Association’s Dementia Practice Care Recommendations. Welsch was the first author on an award-winning abstract describing the program, presented at the Western Institute of Nursing’s April 2024 conference. Read more about the project in the recent
Welsch served as a Person-centered Care Coach on project in Washington State spearheaded by the Alzheimer’s Association. The project aimed to help long-term care facilities improve quality care for people living with Alzheimer’s and dementia by implementing the Alzheimer’s Association’s Dementia Practice Care Recommendations. Welsch was the first author on an award-winning abstract describing the program, presented at the Western Institute of Nursing’s April 2024 conference. Read more about the project in the recent 




















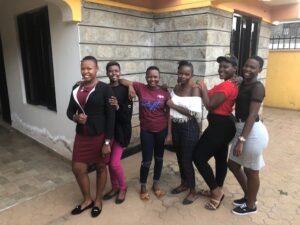


 “As a first-generation Vietnamese immigrant and college student, earning a Bachelor’s degree is more than just fulfilling the American dream. It represents a journey of determination and resilience fueled by the unwavering support from my community. Inspired by those whom I have met along the way and helped me grow into who I am today, I’m committed to doing the same and giving back to others. I plan to pursue pediatric critical care, with the long-term goal of returning to UWSoN to become a nursing educator, where I hope to continue to empower future generations of aspiring leaders in healthcare.”
“As a first-generation Vietnamese immigrant and college student, earning a Bachelor’s degree is more than just fulfilling the American dream. It represents a journey of determination and resilience fueled by the unwavering support from my community. Inspired by those whom I have met along the way and helped me grow into who I am today, I’m committed to doing the same and giving back to others. I plan to pursue pediatric critical care, with the long-term goal of returning to UWSoN to become a nursing educator, where I hope to continue to empower future generations of aspiring leaders in healthcare.”
 The Master of Science Outstanding Student Award is given to the MS student who best exemplifies the program goals: Creativity, Scholarship, Potential in the Profession, and Contributions to the Community
The Master of Science Outstanding Student Award is given to the MS student who best exemplifies the program goals: Creativity, Scholarship, Potential in the Profession, and Contributions to the Community
 Mihkaila Wickline, PhD Student
Mihkaila Wickline, PhD Student
 Lee-Ling Chen is one of the de Tornyay Center for Healthy Aging’s 2023-2024 Healthy Aging Doctoral Scholars, and a UW School of Nursing Adult Gerontology Primary Care Nurse Practitioner Doctor of Nursing Practice student. Her project is on “Fall Prevention and Management for Older Adults in Assisted Living Service Programs within Retirement Communities”. Her faculty mentor is Jonathan Auld, PhD, MAT, RN.
Lee-Ling Chen is one of the de Tornyay Center for Healthy Aging’s 2023-2024 Healthy Aging Doctoral Scholars, and a UW School of Nursing Adult Gerontology Primary Care Nurse Practitioner Doctor of Nursing Practice student. Her project is on “Fall Prevention and Management for Older Adults in Assisted Living Service Programs within Retirement Communities”. Her faculty mentor is Jonathan Auld, PhD, MAT, RN.









 Emilie Martel-Rousseau is a DNP student in the Adult-Gerontology Primary Track and the de Tornyay Center for Healthy Aging’s 2023-2024 Myrene C. McAninch Doctoral Scholar. Her mentor is Assistant Professor Maya Elias and her de Tornyay Center research project is the “Dementia Action Collaborative Provider Survey.”
Emilie Martel-Rousseau is a DNP student in the Adult-Gerontology Primary Track and the de Tornyay Center for Healthy Aging’s 2023-2024 Myrene C. McAninch Doctoral Scholar. Her mentor is Assistant Professor Maya Elias and her de Tornyay Center research project is the “Dementia Action Collaborative Provider Survey.” 


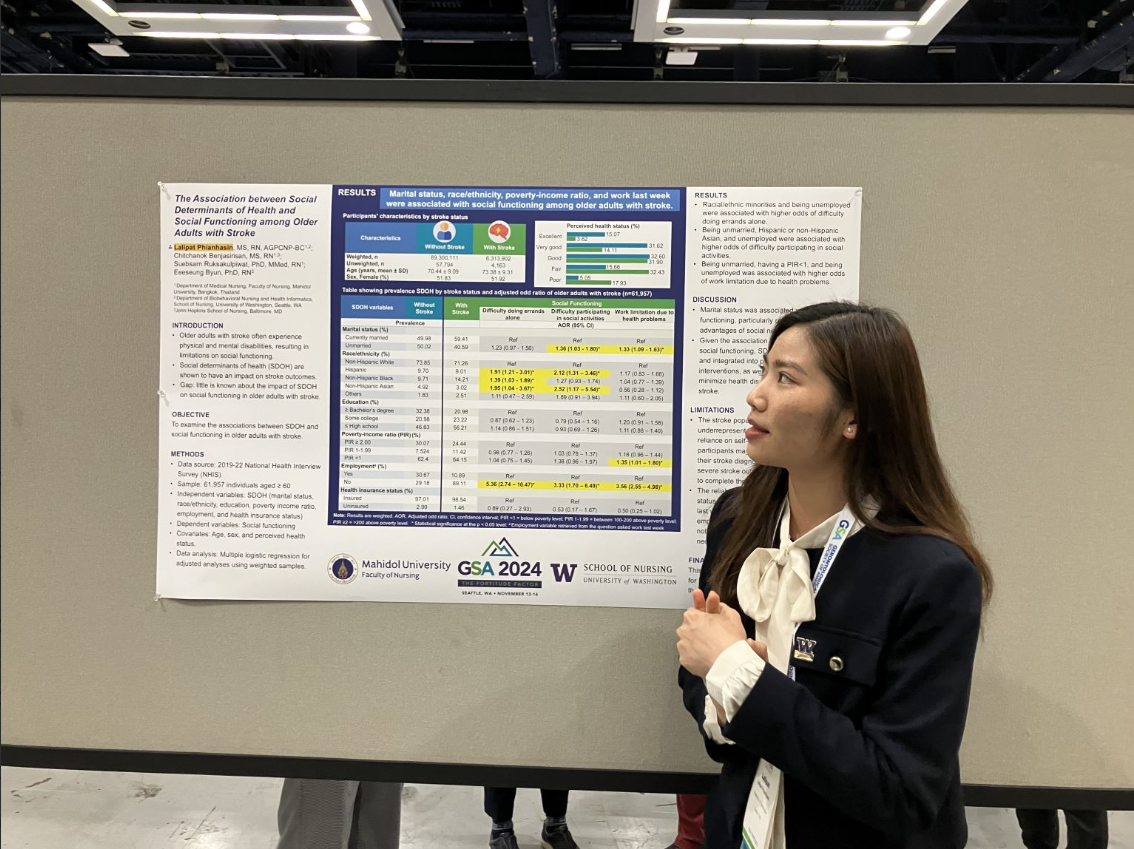
 Lalipat Phianhasin, MS, RN, AGPCNP-BC is a second-year Ph.D. in Nursing Science student and the de Tornyay Center for Healthy Aging illustrator. Her faculty mentor is Dr.
Lalipat Phianhasin, MS, RN, AGPCNP-BC is a second-year Ph.D. in Nursing Science student and the de Tornyay Center for Healthy Aging illustrator. Her faculty mentor is Dr. 

 Yanjing Liang is a first year PhD student and one of the de Tornyay Center for Healthy Aging’s predoctoral scholars. Her research areas of interest include aging-related medical issues.
Yanjing Liang is a first year PhD student and one of the de Tornyay Center for Healthy Aging’s predoctoral scholars. Her research areas of interest include aging-related medical issues.






 Wonkyung Jung
Wonkyung Jung
 Jaemie Lam is a BSN student. During winter quarter in 2023, she traveled to Japan as part of the Keio University Short-Term Nursing and Medical Care Studies Program to learn about challenges of an aging society. UW students attending the program were supported by the Center for Global Health Nursing and the de Tornyay Center for Healthy Aging.
Jaemie Lam is a BSN student. During winter quarter in 2023, she traveled to Japan as part of the Keio University Short-Term Nursing and Medical Care Studies Program to learn about challenges of an aging society. UW students attending the program were supported by the Center for Global Health Nursing and the de Tornyay Center for Healthy Aging. CJ Rivera is a BSN student. During winter quarter in 2023, she traveled to Japan as part of the Keio University Short-Term Nursing and Medical Care Studies Program to learn about challenges of an aging society. UW students attending the program were supported by the Center for Global Health Nursing and the de Tornyay Center for Healthy Aging.
CJ Rivera is a BSN student. During winter quarter in 2023, she traveled to Japan as part of the Keio University Short-Term Nursing and Medical Care Studies Program to learn about challenges of an aging society. UW students attending the program were supported by the Center for Global Health Nursing and the de Tornyay Center for Healthy Aging.

 Dariga Tugan is an ABSN student and one of the de Tornyay Center’s 2022-2023 Healthy Aging Undergraduate Scholars. Her project is “A descriptive analysis of variability in exercise (VO2 Max) to address differences in physical function and alleviation of symptoms in older adults living with HIV”. Her faculty mentor is Dr. Allison Webel.
Dariga Tugan is an ABSN student and one of the de Tornyay Center’s 2022-2023 Healthy Aging Undergraduate Scholars. Her project is “A descriptive analysis of variability in exercise (VO2 Max) to address differences in physical function and alleviation of symptoms in older adults living with HIV”. Her faculty mentor is Dr. Allison Webel.

 Lia Kaluna is the de Tornyay Center for Healthy Aging’s 2021-2022 Germaine Krysan Undergraduate Scholar. A fourth year BSN student, her project is Identifying Key Landmarks of Central District’s Historically Black Neighborhoods. The project is a part of the Seattle SHARP study. SHARP Portland was originally developed by Raina Croff, PhD, an anthropologist at Oregon Health State University. A local team is now developing SHARP Seattle based on the findings from Dr. Croff and her team. Kaluna’s faculty mentor is Dr. Basia Belza.
Lia Kaluna is the de Tornyay Center for Healthy Aging’s 2021-2022 Germaine Krysan Undergraduate Scholar. A fourth year BSN student, her project is Identifying Key Landmarks of Central District’s Historically Black Neighborhoods. The project is a part of the Seattle SHARP study. SHARP Portland was originally developed by Raina Croff, PhD, an anthropologist at Oregon Health State University. A local team is now developing SHARP Seattle based on the findings from Dr. Croff and her team. Kaluna’s faculty mentor is Dr. Basia Belza.

 Dr. Ethlyn McQueen-Gibson serves as an associate professor at the Historically Black College & University (HBCU) Hampton University School of Nursing in Hampton, VA, and the inaugural Director for the Gerontology Center for Excellence & Minority Aging. Prior to assuming the role at Hampton University, she spent two years at Virginia Commonwealth University (VCU) in Richmond in a dual role as part of the Institute of Inclusion, Inquiry and Innovation through the Office of Diversity and the School of Nursing.
Dr. Ethlyn McQueen-Gibson serves as an associate professor at the Historically Black College & University (HBCU) Hampton University School of Nursing in Hampton, VA, and the inaugural Director for the Gerontology Center for Excellence & Minority Aging. Prior to assuming the role at Hampton University, she spent two years at Virginia Commonwealth University (VCU) in Richmond in a dual role as part of the Institute of Inclusion, Inquiry and Innovation through the Office of Diversity and the School of Nursing.