Courses & registration
Curriculum grids
Undergraduate degree programs
| Program | Cohort start year |
|---|---|
| Bachelor of Science in Nursing (BSN) | 2018 | 2019 | 2020 or 2021 | 2022 | 2023 |
| Accelerated Bachelor of Science in Nursing (ABSN) | 2021 | 2022 2023: Spring | Autumn |
Graduate degree programs
| Program | Cohort start year |
|---|---|
| Master of Science: Clinical Informatics and Patient-Centered Technologies (CIPCT) | 2020: Full-time | Part-time 2021: Full-time | Part-time |
| Doctor of Nursing Practice: Adult-Gerontology Acute Care Nurse Practitioner (AGNP-AC) | 2021 | 2022 | 2023 | 2024 |
| Doctor of Nursing Practice: Adult-Gerontology Primary Care Nurse Practitioner (AGNP-PC) | 2020 | 2021 | 2022 | 2023 | 2024 |
| Doctor of Nursing Practice: Family Nurse Practitioner (FNP) | 2019 | 2020 | 2021 | 2022 | 2023 | 2024 |
| Doctor of Nursing Practice: Nurse-Midwifery (NM) | 2021 | 2022 | 2023 | 2024 |
| Doctor of Nursing Practice: Pediatric Clinical Nurse Specialist (PCNS) | 2021 | 2022 | 2023 | 2024 |
| Doctor of Nursing Practice: Pediatric Nurse Practitioner Acute Care (PNP-AC) | 2021 | 2022 | 2023 | 2024 |
| Doctor of Nursing Practice: Pediatric Nurse Practitioner Primary Care (PNP-PC) | 2020 | 2021 | 2022 | 2023 | 2024 |
| Doctor of Nursing Practice: Population Health & Systems Leadership (PHSL) | 2021 | 2022 | 2023 | 2024 |
| Doctor of Nursing Practice: Psychiatric Mental Health Nurse Practitioner (PMHNP) | 2018 | 2019 | 2020 | 2021 | 2022 | 2023 | 2024 |
| Doctor of Nursing Practice: Women’s Health Clinical Nurse Specialist (WHCNS) | 2021 | 2022 | 2023 | 2024 |
| Doctor of Philosophy in Nursing Science (PhD) | 2019 and earlier | 2020 and later EDPSY sequencing combinations PhD Required and Elective Courses |
Graduate certificate programs
| Adult-Gerontology Acute Care Nurse Practitioner Certificate (AGNP-AC) | Download grid |
| Adult-Gerontology Primary Care Nurse Practitioner Certificate (AGNP-PC) | Download grid |
| Advanced Practice Environmental and Occupational Health (APEOH) | Download course requirements Sample Work and Health Curriculum 1 Sample Work and Health Curriculum 2 |
| Global Health Nursing | Sample curriculum grids |
| Nurse-Midwifery | View course requirements |
| Palliative Care (PC) | Download grid |
Registration process
Accelerated Bachelor of Science in Nursing
ABSN students register through MyUW.
Bachelor of Science in Nursing
BSN students follow the registration process administered by the UW Office of the Registrar.
Doctor of Nursing Practice: Fee-based programs
Programs include:
- Adult-Gerontology Acute Care Nurse Practitioner
- Adult-Gerontology Primary Care Nurse Practitioner
- Family Nurse Practitioner
- Nurse-Midwifery
- Women’s Health Clinical Nurse Specialist
Doctor of Nursing Practice: State tuition-based programs
Programs include:
- Pediatric Clinical Nurse Specialist
- Pediatric Nurse Practitioner, Acute Care
- Pediatric Nurse Practitioner, Primary Care
- Population Health & Systems Leadership
- Psychiatric Mental Health Nurse Practitioner
Doctor of Philosophy in Nursing Science
PhD students follow the registration process administered by the UW Office of the Registrar.
Graduate certificate programs: Fee-based programs
Programs include:
- Adult-Gerontology Acute Care Nurse Practitioner
- Adult-Gerontology Primary Care Nurse Practitioner
- Nurse-Midwifery
- Women’s Health Clinical Nurse Specialist
Graduate certificate programs: State tuition-based programs
Programs include:
- Advanced Practice Environmental and Occupational Health
- Pediatric Clinical Nurse Specialist
- Pediatric Nurse Practitioner, Acute Care
- Pediatric Nurse Practitioner, Primary Care
- Psychiatric Mental Health Nurse Practitioner
Graduate non-matriculated status
You will receive guidance about how to register as a GNM student for your course(s) when you are admitted to the UW School of Nursing.
GNM students who have permission to take a course and are not using a tuition exemption benefit will register before the start of the quarter of admission by submitting forms to the UW Non-Degree Enrollment Office, located off-campus in the University District.
A tuition-exempt GNM student with permission to take a course from a non-fee-based program will register on the third or fourth day of the quarter as outlined in the UW State Employee Tuition Exemption guidelines. Please note you must have already received student status to take advantage of the tuition exemption benefit.
Master of Science: Clinical Informatics and Patient-Centered Technologies
MS-CIPCT students register through MyUW.
Degree requirements
Master of Science: Clinical Informatics and Patient-Centered Technologies
The estimated length of time required to complete the Clinical Informatics and Patient-Centered Technology Master of Science program is 15 months of full-time study. Part-time study is available.
Goals of the Master of Science program
- Evaluate the current state of knowledge in a selected area of clinical informatics as it informs theory, practice, and research.
- Develop and implement scholarly inquiry related to clinical informatics or patient-centered technology.
- Articulate ethical issues, practical challenges, and responsibilities involved in collecting and managing data to generate new knowledge.
- Develop and utilize organization and system leadership strategies that foster innovation and improvement of health care.
- Design, implement and utilize healthcare technologies to promote quality of care, patient engagement and safety, as well as clinical and cost-effectiveness.
Minimum school requirements: Master of Science
| Course | Credits | Quarter |
| Informatics Courses | ||
| NMETH 527 Intro to Clinical Informatics | 3 | Autumn |
| NMETH 528 Computing Fundamentals for Health Professionals | 3 | Winter |
| NMETH 529 Database Concepts & Applications in Clinical Informatics | 3 | Spring |
| NMETH 523 Project Management and Systems Analysis for Health Informatics | 3 | Autumn |
| NMETH 524 Healthcare Information Systems & the EHR | 3 | Winter |
| NMETH 526 Patient-Centered Technologies | 3 | Spring |
| NSG 540 Telehealth | 4 | Summer |
| Care Systems Courses |
||
| NURS 524 Health Systems: Organizational Structure and Effectiveness | 4 | Autumn |
| NURS 525 Managing Quality Improvement, Access, and Utilization | 5 | Winter |
| Scholarly Inquiry Courses | ||
| NMETH 520 Scholarly Inquiry for Clinical Informatics Practice | 4 | Spring |
| NMETH 530 Scholarly Proposal Development | 4 | Summer |
In addition to the above required courses, students are required to complete a Scholarly Project.
Doctor of Nursing Practice
The Doctor of Nursing Practice program is focused on preparing advanced practice nurses in accordance with the American Association of Colleges of Nursing (AACN) Essentials of Doctoral Education for Advanced Nursing Practice. The term Advanced Practice refers to any form of nursing intervention that influences health care outcomes for individuals or populations. This includes:
- the direct care of individual patients
- management of care for individuals and populations
- administration of nursing and health care organizations, and
- the development and implementation of health policy
Preparation at the practice doctorate level, including advanced preparation in nursing, is based on nursing science and is at the highest level of nursing practice. Advanced practice, practice inquiry, and leadership are the major themes of the curriculum. Domain threads integrated into core courses include:
- ethics
- informatics
- communication, and
- interprofessional training
The graduate faculty in the School of Nursing approved revised DNP program goals, core elements, and a conceptual model for a consolidated curriculum in 2012. The goals are based on the DNP program goals adopted by SON faculty in December 2008 but broadened to reflect the scope of advanced nursing practice preparation to include community health perspectives on population health, systems of care, prevention, and social justice
The curriculum also aligns with the national Licensure Accreditation, Certification, and Education (LACE) model for students seeking preparation as nurse practitioners (NP), clinical nurse specialists (CNS) and nurse midwives (NM). Core elements identify the DNP program as a core program of the SON, all students have the same number of required credits (minimum of 93), and the majority of courses are required of all students.
The DNP is conceptualized as a single degree from the SON with multiple specialty tracks organized within the degree. Two major branches of the program identified are the Advanced Practice Registered Nursing (APRN) and Advanced Systems and Population Health (ASPH), each with specific core coursework. The program culminates with a final project and an immersive clinical experience during which the student is expected to demonstrate the expected end of program competencies in advanced practice, leadership and practice inquiry (tripartite role).
Applicants are evaluated for fit with the DNP degree and fit with the specialty track.
Program curriculum model: “The Dawg Path”
The figure below, which we call the Dawg path, shows the conceptualization of the program, delineating the basic and advanced DNP core, the APRN and ASPH cores, and the shared/ unique specialty courses.
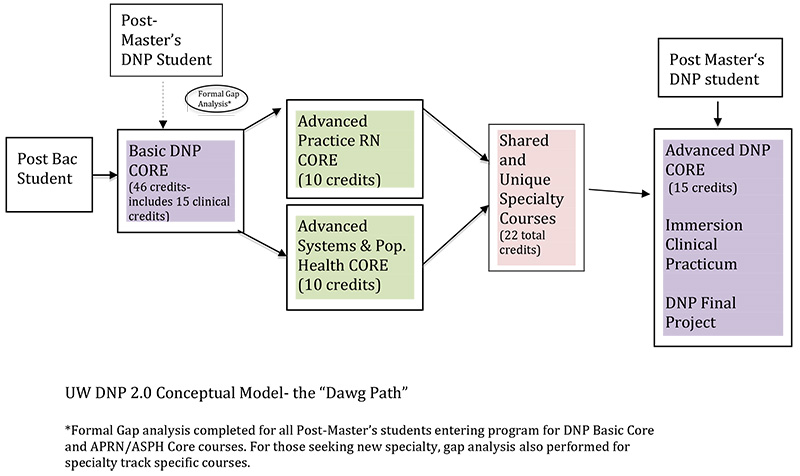
Basic DNP core
The DNP Year 1 core courses focus on the DNP role and foundational content since this is the degree to which all students are admitted. The emphasis is on the commonalities among all the students as learners; however, learning activities in the first year will also introduce students to their specialty track.
Beginning the curriculum with DNP Core courses assists students to affirm their interest in and ability to continue in the program before they begin the specialty track training.
These Year 1 courses are required of and taken by all students for the DNP degree. The objectives of these courses meet the DNP Essentials (2006) I-VIII. [Coded Purple]
APRN and ASPH core
APRN Core is required of all students preparing for advanced practice registered nurse certification and licensure roles (i.e., NP, CNS, CNM). These courses meet the “3 P’s as outlined in the LACE consensus document: advanced physical assessment, advanced pharmacology, advanced pathophysiology.” [Coded Green]
ASPH Core is required of all students preparing for the advanced systems & population health track. (Currently only Population Health in this branch) [Coded Green]
Specialty Didactic and Clinical Courses include additional coursework necessary to meet certification requirements (if appropriate) for individual specialty tracks. Each track includes a series of 3 clinical practica courses (a fourth clinical course is included in the final project).
Advanced DNP core: the final project and clinical immersion
Advanced DNP Core includes 2 courses focused on the DNP project and a clinical immersion course. The foundations for the DNP project occur during Year 1 with the series of practice inquiry courses.
In the final two quarters of the curriculum, two courses are focused on the DNP final project. The first course is focused on planning practice inquiry and systems-level change projects, and the second course is focused on the implementation and evaluation of the project in a clinical setting.
The combination of the project implementation course with the clinical immersion course in the final quarter is intended to provide an opportunity for synthesis of advanced practice, practice inquiry, and leadership and also to serve as a transition to advanced practice as a DNP-prepared practitioner.
The clinical immersion course consists of 9 credits and the student averages 3 days a week in the clinical setting.
Doctor of Philosophy in Nursing Science: Cohorts beginning autumn 2019 and earlier
Expected student outcomes
The program has a required minimum of 93 quarter credits for completion, and graduates must meet five expected student outcomes:
- generate knowledge that is inventive and rigorously tested within a selected area of nursing science;
- have multiple perspectives of knowing and also acknowledge multidisciplinary contributions to knowledge generation;
- be informed by social, cultural and political issues related to their area of scholarship;
- provide leadership in nursing as well as various professional and public groups;
- test, generate and extend knowledge relevant to nursing science and practice.
Course/credit requirements
We anticipate that the average student will exceed the required number of credits by adding courses that provide knowledge that is unique to their area of research interest. Each student’s supervisory committee has the final responsibility for approving his or her program of study.
Of the 93 credits required for graduation, 41 credits are defined as Theory and Domain of Knowledge, and 52 credits are defined as Scholarly Inquiry.
DOWNLOAD THE SAMPLE PHD PROGRAM SCHEDULE
ADDITIONAL LEARNING OPPORTUNITIES: SCHOOL OF NURSING CENTERS
Theory and Domain of Knowledge
Minimum 41 credits
Courses included in the Theory and Domain of Knowledge requirements focus on individual, family and community interactions with supporting and non-supporting environments that result in human behavioral responses and adaptation to wellness and illness. Variations in human responses and adaptation are influenced by many factors such as biology, gender, age, social class, and culture.
*Required (core) courses are highlighted in bold.
Course |
Credits |
|---|---|
| NURS 587: Role Transition Seminar | 2 |
| NURS 588: Philosophical Basis of Nursing Inquiry | 3 |
| NURS 589: Theoretical Perspectives in Nursing Science | 3 |
| NURS 590: Ecology of Human Health | 5 |
| NURS 592: The Science of Therapeutics: Theoretical Foundations | 4 |
| NURS 595: Synthesis of Nursing Science | 3 |
| Graduate Nursing Courses | 9 |
| Related Fields: Courses without an NSG, NURS, NCLIN, or NMETH prefix; may be independent study | 12 |
Scholarly Inquiry
Minimum 52 credits
Courses included in the Scholarly Inquiry requirements focus on research methodologies and research methods to develop knowledge. Students learn a variety of methodologies with encouragement to develop advanced skills in at least one methodology. Courses in this category are grouped into three required sub-categories:
- *Core Methods Courses (11 credits)
These courses give students an overview of research design, methods, and data analyses.
Course |
Credits |
|---|---|
| NMETH 579: Research Design and Methods | 4 |
| NMETH 580: Methodological Perspectives in Nursing Science | 3 |
| NMETH 591: The Science of Therapeutics: Design and Outcomes | 4 |
- Design/Methods/Statistics (14 credits)
These courses allow students to obtain in-depth knowledge of research designs, methods, and statistical approaches.
In addition to the courses listed below, the Department of Biostatistics offers many interdisciplinary research methods and statistical courses.
Advanced Methods: 4 Credits Minimum
Courses meeting the Advanced Methods requirement are not limited to nursing courses.
Course |
Credits |
|---|---|
| EDPSY 588: Survey Research Methods | 3 |
| EDLPS 574: Mixed Methods in Educational Research | 3 |
| NMETH 584: Methods: Physiological Measures | 4 |
| NMETH 590: Qualitative Inquiry | 2-5 |
| BIOST 524: Design of Medical Studies | 3 |
Statistics: 10 Credits Minimum
Beginning Fall 2019, EDPSY490 is not eligible to count as part of the required statistics credits. Students should identify an appropriate sequence of courses with the assistance of their adviser/chair to meet this requirement to ensure developing competency in statistical analysis.
Statistics Courses |
Credits |
|---|---|
| BIOST 511: Medical Biometry I | 4 |
| BIOST 512: Medical Biometry II | 4 |
| BIOST 513: Medical Biometry III | 4 |
| EDPSY 593: Experimental Design and Analysis (with permission of instructor) | 5 |
| EDPSY 594: Advanced Correlational Techniques (with permission of instructor) | 5 |
| PSYCH 525: Linear Models and Data (with permission of instructor) | 4 |
| SOC 504: Applied Social Statistics (with permission of instructor) | 3 |
| SOC 505: Applied Social Statistics (with permission of instructor) | 3 |
Advanced Statistic Courses |
Credits |
|---|---|
| BIOST 524: Design of Medical Studies | 3 |
| EDPSY 575: Structural Equation Modeling | 3 |
| EDPSY 576: Hierarchical Linear Models/Multilevel Modeling | 3 |
| SOC 526: Causal Approach to Theory Building and Data Analysis (with permission of instructor) | 3 |
| SOC 529: Structural Equation Models for the Social Sciences (with permission of instructor) | 3 |
| Courses Offered by the Center for Statistics and the Social Sciences (CSSS) | Credits vary |
- Dissertation: NMETH 800 (27 credits)
Doctor of Philosophy in Nursing Science: Cohorts beginning autumn 2020 and later
Expected student outcomes
- Have multiple perspectives of knowing and acknowledge multidisciplinary contributions to knowledge generation
- Demonstrate substantive knowledge within a particular area of nursing science with particular emphasis on issues and questions within the field that require scholarly attention
- Innovate and rigorously test, generate and extend knowledge in an area relevant to nursing science
- Communicate, disseminate, and critique nursing science and scholarly activities in both oral and written formats
- Demonstrate critical interrogation of positionality, recognition of implicit biases, as well as knowledge and application of anti-racism principles to promote health equity.
Course/credit requirements
Course type |
Credits |
|---|---|
| Nursing Science Core | 29 |
| Statistics Sequence | 12 (minimum) |
| Epidemiology | 4 (minimum) |
| Clinical Trials | 3 (minimum) |
| Policy | 2 (minimum) |
| Advanced Nursing Science or Nursing Methods Electives | 6 (minimum) |
| Related Fields (non-nursing) | 6 (minimum) |
| Teaching Practicum | 3 |
| Research Practicum | 4 |
| Dissertation | 27 |
| TOTAL | 96+ |
Doctor of Philosophy in Nursing Science statistics concentration (all cohorts)
This area of concentration is offered by the School of Nursing in collaboration with the Center for Statistics and the Social Sciences (CSSS). This is a program option that offers the opportunity for advanced training in statistical methods to complement your PhD program of study. Successful completion of the statistics concentration is recognized by the University of Washington and is recorded on your transcript as part of your PhD degree.
The area of concentration includes four additional advanced statistical methods courses and at least two quarters of CS&SS 590, the weekly CSSS Seminar. These courses are above and beyond the 12 credits of advanced statistics required for all PhD students. You must receive numerical grades for all courses taken as part of the statistics concentration.
Requirements and process
If you are interested in the statistics area of concentration, you should speak to the Chair of your PhD Supervisory Committee. You will need to work with your chair and your supervisory committee members to develop a Statistics Area of Concentration Coursework Proposal as part of your overall Program of Study.
To begin work in this statistics area of concentration, you must meet the following requirements:
- You must have completed the basic statistical and methodological course requirements for the PhD program.
- Your supervisory committee must be established, and include one member related to the statistics area of concentration: a School of Nursing graduate faculty member who is currently teaching quantitative methodology in nursing; a School of Nursing faculty member who is also a CSSS affiliate faculty member; and/or a core faculty member from CSSS.
- If your program of study has already been approved by your supervisory committee, you will need to submit a revised program of study to Student and Academic Services.
Statistics area of concentration coursework proposal
Your Coursework Proposal describes your course work’s relevance to the statistics area of concentration, and should contain the following elements:
- At least two quarters of CS&SS 590: CSSS Seminar.
- At least four additional advanced statistics courses for a minimum of 12 credits; at least three of the courses must be selected from the CSSS list of approved courses for the nursing concentration.
- The rationale for the selection of specific courses.
- The proposed sequence (quarter and year) in which you will take each statistics course.
- A letter notifying the CSSS Director of your intention to pursue the concentration.
Completing the concentration
Successful completion of the program will be based on:
- Completion of a minimum of 12 credits from at least four advanced statistical courses described and justified in the approved Area of Concentration Coursework Proposal. At least three of the courses should be CSSS 500-level courses.
- A grade of 3.3 or greater in each course designated in the area of concentration.
- Participation in at least two quarters of the CSSS Seminar, CS&SS 590.
- Upon completion of all courses and the seminar. You must submit summaries of courses completed, course syllabi, grades, and any relevant assignments, including papers or projects to your PhD Supervisory Committee for review.
- The completed program is also submitted to the CSSS Director.
Your committee will review your coursework, and your chair will inform you in writing whether or not you have successfully completed the Nursing Science Statistics Area of Concentration.
The Nursing Science Statistics Area of Concentration requires a minimum of fourteen credits of advanced statistical methods coursework above and beyond the 12 credits of statistics required for the PhD degree. Of these, two credits are fulfilled by the CSSS Seminar, and a minimum of 12 credits are fulfilled by at least four advanced statistics courses, three of which must come from the list of CSSS courses approved for the concentration.
All courses taken as part of the statistics concentration must be graded.*
CSSS seminar: minimum of two credits
A minimum of 2 quarters in CS&SS is required. The most up-to-date course descriptions for statistics course options can be found on the CSSS website.
| Course | Credits |
|---|---|
| CS&SS 590: CSSS Seminar | 1 |
Approved CSSS advanced statistics course options
The most up-to-date course descriptions for statistics course options can be found on the CSSS website.
| Course | Credits |
|---|---|
| CS&SS 510: Maximum Likelihood Methods for the Social Sciences | 5 |
| CS&SS 526: Structural Equation Models for the Social Sciences | 3 |
| CS&SS 527: Survey Research Methods | 4 |
| CS&SS 529: Sample Survey Techniques | 3 |
| CS&SS 536: Analysis of Categorical and Count Data | 3 |
| CS&SS 544: Event History Analysis for the Social Sciences | 5 |
| CS&SS 560: Hierarchical Modeling for the Social Sciences | 4 |
| CS&SS 564: Bayesian Statistics for the Social Sciences | 4 |
| CS&SS 565: Inequality: Current Trends and Explanations | 3 |
| CS&SS 566: Causal Modeling | 4 |
| CS&SS 567: Statistical Analysis of Social Networks | 4 |
| CS&SS 568: Game Theory for Social Scientists | 5 |
| CS&SS 589: Multivariate Data Analysis for the Social Sciences | 3 (max. 6) |
| CS&SS 592: Applied Longitudinal Data Analysis for Social Sciences | 4 |
| CS&SS/SOC WL 594: Longitudinal Data Analysis | 1-5 |
Variation in area of concentration coursework
One advanced methodological course in nursing, political science, psychology, public health, sociology, statistics, economics, educational psychology, social welfare, and other related fields may be considered as part of the Nursing Science Statistics Area of Concentration four course requirements, if it contributes to the overall coherence of the student’s program of study and is consistent with the student’s research goals. Such a course would be in addition to the ten credits of statistics courses required for the PhD in nursing.
*A 500-level course that is graded credit/no credit may be considered for inclusion in your Area of Concentration proposal if:
- In the course, you submit an individual project [i.e., not a group project]; and
- Major course assignments are submitted to your Supervisory Committee for review
Program of study
Your program of study consists of core program requirements plus courses recommended by your adviser or supervisory committee based on your interests.
Doctor of Nursing Practice: Cohorts beginning autumn 2017 and earlier
Developing your program of study
- Beginning the first quarter of your doctoral program, you should maintain an ongoing program of study listing the courses you are taking and plan to take using the approved form for your track.
- Once your Supervisory Committee has been appointed, you will work with your committee to finalize the program of study and submit the form to your supervisory committee for formal review and approval (Autumn Quarter Year 3).
- After your supervisory committee approves your program of study, you must submit a signed hard copy and electronic copy to Student and Academic Services for your student file.
Guidelines for approval of the program of study
The Supervisory Committee evaluates the proposed program of study using the following guidelines:
- Are all program and track requirements met? Does the program of study comply with all University rules and regulations?
- Is it feasible to implement and complete the program of study in a timely manner?
- If courses were taken at another university or for another program of study (e.g., master’s degree) are included in the program of study, is there an approved gap analysis and approval from DNPCC on file?
Doctor of Nursing Practice: Cohorts beginning autumn 2018 and later
Select the appropriate DNP grid for your track and entry year from the DNP Program Courses & Registration page.
Completing the program of study as-is
If you are completing the program of study for your track as per the grid (no course substitutions or waivers), upload this form to Canvas. (Do not worry about elective courses.)
Completing the program of study with substituted/waived courses
If you are not completing the program of study for your track exactly as per the grid (e.g., you have substituted or waived classes), you must also upload an Exceptions Addendum with your grid when requested during NMETH 801 to the Canvas site. In this “Exceptions Addendum,” please identify which courses you did not take, and what course(s) from what universities/colleges are substituting for that course.
- Prior to uploading the Addendum, please make sure that you have had your track lead/advisor review it for accuracy.
- Save file: Trackprogramofstudy_FirstLastname_date (example: PCNSprogramofstudy_SueSmith_December-2020)
- Save addendum: Exceptionaddendum_FirstLastname_date (example: Exceptionaddendum_SueSmith_December-2020)
The program of study forms will then be reviewed and submitted to Student and Academic Services.
Doctor of Philosophy in Nursing Science
The program of study is a written description, by each doctoral student in communication with the faculty adviser initially, and then with the supervisory committee, of:
- the substantive emphasis of the courses taken or planned, including the emphasis in nursing theory and the related field selected;
- the outcomes of each course; and
- the inquiry focus for the doctoral dissertation.
- Developing your program of study
- Guidelines for approval of the program of study
- What to include in the program of study
- Considerations for developing your program of study
- Sample program of study
Developing your program of study
- Beginning the first year of the doctoral program, an ongoing program of study is to be completed each quarter by the student. Students must consider far in advance if they would like to petition for previous coursework equivalency.
- Once the student’s supervisory committee has been appointed, the program of study functions as an initial draft to the committee, to be used for planning future course needs and learning.
- The program of study is then submitted by the student for formal review to the entire supervisory committee, including the Graduate School Representative, along with a statement of research interest.
- Using a set of prescribed guidelines, the supervisory committee conducts a formal review of the program of study, making any suggestions for modifications prior to approval.
- Following the supervisory committee’s approval, the program of study is submitted to Student and Academic Services (SAS) for placement in the student’s file, accompanied by a formal letter of approval by the chair of the committee.
Guidelines for approval of the program of study
The supervisory committee evaluates the proposed program of study using the following guidelines:
- Does the coursework support the student’s substantive emphasis on theory and knowledge development?
- What is the content and scope of plans for guided scholarship/independent study? Is adequate “guidance” available?
- Are the related courses logically consistent for the described program of study?
- Are the statistics and methods courses adequate to prepare the student for the conduct of the dissertation?
- How has the Program of Study enabled the student to strengthen reasoning, writing and communication skills?
- What is the degree of exposure of the student to various faculty expertise across the School and University?
- To what extent does the program provide a) depth of study as well as preparation beyond the single dissertation planned, and b) role development as a researcher and teacher?
- Are all program requirements met? Does the program of study comply with all University rules and regulations?
- Is the program of study feasible to implement and complete in a timely manner?
- If courses are proposed that were taken at another University or for another program of study (a master’s degree, for example), do they represent adequate content? Is the content appropriately current? Do the courses fall within the ten-year limit?
- With what other scholarly work has the student been involved? Has the student been involved in Research or Teaching Assistant activities? Has the student submitted a National Research Service Award application for an Independent Fellowship? Has the student published any articles while in the doctoral program?
What to include in the program of study
- Number, name, and number of credits of each course taken or to be taken;
- The faculty member teaching each course;
- Date course is taken, or proposed schedule;
- Course description and outcomes, such as course product, reasoning skills, communication skills;
- The rationale of each course’s placement within the areas of study as per program requirements;
- The rationale for how the contents of a course taken prior to admission support the program of study;
- Space for signature and date of the supervisory committee chair and each supervisory committee member attesting to their approval of the program of study.
Considerations for developing your program of study
Course load and credits
Ten credits are considered a full-time course load. Each doctoral student must have completed the required number of program credits, sixty of which must have been completed in residency at the University of Washington, in order to earn the doctoral degree.
Academic progress and scholarship
A cumulative grade point average of 3.0 or better is required for completion of any graduate program at the University of Washington. A minimum of 2.7 is required in each of the required nursing core courses.
Course scheduling
The majority of required courses are offered in the academic year, autumn through spring quarter. All required courses, exclusive of the dissertation, can be completed in two years of full-time study. As the majority of students enrolled in the program work concurrently with their course work, nursing core courses are arranged to consolidate offerings to two to three days during the week. We do not recommend working over twenty hours per week while in the program. Some scholarships, loans, and research or teaching assistantships are available.
Faculty availability
Most School of Nursing faculty have nine-month appointments, and may or may not be teaching in summer quarter.
Independent study
NURS 599: Selected Readings is defined as an individual reading or work on a paper with a faculty member. NMETH 600: Guided Scholarship is defined as individual work on a research project (not the dissertation) in which manipulation of data is included. A form stating an agreement between the faculty member and the student as to the purpose of the study is required before enrolling in either of these independent study options. These courses differ from NMETH 610 Research Practicum in which a student embeds with an active research team and works in collaboration with them, reflecting on team science. Forms are available in SAS and must be returned to SAS for your file when the study experience has been completed.
Previous credits
Although the University does not accept transfer credits into the doctoral program, up to thirty credits of graduate course work taken as part of a master’s program may be requested to meet part of the nursing or the related fields requirement. Such courses must be directly relevant to the student’s area of research and have been taken within the previous ten years. The Supervisory Committee approves such requests when it approves the student’s program of study. The approved program of study is then forwarded to SAS for the student file.